Graves’ Disease causes hyperthyroidism (overactive thyroid gland), weight loss, anxiety & fatigue. Find out more about the causes of Graves’ Disease, associated health issues, and treatments.
What is Graves’ Disease?
Graves’ disease is an autoimmune disease that increases the activity of the thyroid, a small gland in the neck, resulting in overproduction of thyroid hormones [1, 2].
It is caused by thyroid stimulating immunoglobulins (TSI), also known as thyroid stimulating antibodies (TSAb) or thyroid receptor antibodies (TRAb). These antibodies impersonate thyroid stimulatory hormone (TSH) normally produced by the pituitary gland, stimulating the production of thyroid hormones T4 and T3 [1].
Graves’ disease is the most common cause of hyperthyroidism (overactive thyroid) in the world, accounting for 70-80% of hyperthyroid cases [1, 2, 3].
Symptoms
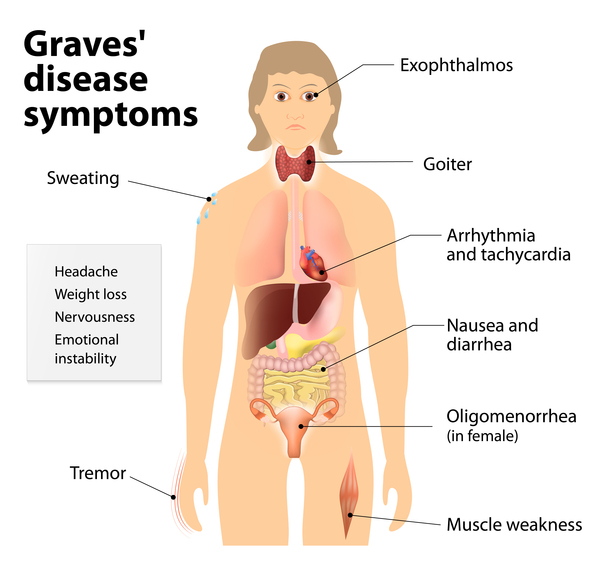
Thyroid hormones affect pretty much all other organs in the body by adjusting how fast metabolism works. That’s why symptoms associated with Graves’ disease can be many and diverse. Common signs and symptoms include [2, 4]:
- Weight loss
- Anxiety and irritability
- Increased heart rate
- Fatigue
- Tremors
- Sensitivity to heat
- Enlarged thyroid gland (swollen neck)
- Irregular periods
- Eye pain and redness
- Swollen and protruded eyeballs (Graves’ ophthalmopathy)
- Thick, red skin on the shins or feet (Graves’ dermopathy)
- Dermopathy (skin disease)
These symptoms are not unique, many other conditions can cause them. If you are experiencing any of these symptoms, work with your doctor as soon as possible to get an accurate diagnosis.
Seek immediate care if you’re experiencing heart-related symptoms or vision loss!
Diagnosis
To help diagnose Graves’ disease, doctors will look at a number of things, including your signs and symptoms and blood tests, including [2]:
- TSH
- Thyroxine (T4)
- Triiodothyronine (T3)
People with Graves’ disease usually have high levels of thyroid hormones (T4 and T3) and low levels of thyroid stimulating hormone (TSH) [2].
If needed, your doctor can also check [2]:
- levels of antibodies that cause Graves’ disease (TRAb test)
- radioactive iodine uptake
- if the thyroid gland is enlarged by ultrasound or imaging tests (CT, MRI)
Understanding your risk for Graves’ disease can provide valuable insights into your thyroid health. By examining both genetic and lifestyle factors, you can gain a clearer picture of your likelihood of developing this condition. SelfDecode’s Longevity Screener test helps you explore these risks, supporting informed decisions to maintain your overall well-being.
Causes and Mechanisms
Specific immunoglobulins (IgG antibodies), called thyroid stimulating immunoglobulin (TSI), thyroid stimulating antibodies (TSAb), or thyroid receptor antibodies (TRAb), bind to and activate the thyroid stimulating hormone (TSH) receptor on thyroid gland cells. This causes thyroid gland cell growth, which results in an enlarged thyroid and high thyroid hormone levels [4].
A study suggests that Th17 and Th22 cells may play a role in Graves’ disease development by increasing the autoimmune response [5].
Risk Factors
Although anyone can develop Graves’ disease, there are a number of factors that can increase the risk. These risk factors include [4, 6]:
- A family history of Graves’
- Female gender
- Being under 40
- Having other autoimmune disorders (e.g. type 1 diabetes, rheumatoid arthritis)
- Emotional or physical stress, such as stressful events or serious illness, may act as triggers
- Pregnancy and recent childbirth
- Smoking
The overall prevalence of hyperthyroidism in the US is around 1.2% with an incidence of 20/100,000 to 50/100,000. Some data suggest its lifetime risk in women and men is 3% and 0.5%, respectively [1].
Graves’ Disease and Other Health Issues
Graves’ Disease and Ophthalmopathy
This condition occurs in about a third of people who have Graves’ disease. It’s an eye disease that causes the eye to protrude and the eyelids to retract and lag when opening or closing. T cells (white blood cells) in the body attack an antigen (a molecule that causes an immune response) in the eyes. This leads to swelling and eyeball protrusion [7].
People with this condition usually have a sandy sensation in their eyes, blurry vision, infrequent blinking, dry eyes, and irritation [7].
Grave’s ophthalmopathy can, in some cases, occur without hyperthyroidism.
Graves’ Disease and Dermopathy
Dermopathy is a skin condition that causes the skin to become red and thick, resembling that of an orange [7].
This manifestation is relatively uncommon.
Graves’ Disease and Pregnancy
In pregnant women with Graves’ disease, the antibodies can cross the placenta and also cause thyroid dysfunction in the fetus [8].
Because Graves’ is an autoimmune disease, it can be problematic during the early stages of pregnancy. However, during pregnancy, the immune system is suppressed and Graves’ can improve [8].
If hyperthyroidism and Graves’ is unmanaged, it can cause problems such as [8]:
- High blood pressure
- Heart failure
- Miscarriage/stillbirth
- Premature birth
- Fetus abnormalities
Grave’s Disease and Osteoporosis
Excessive amounts of thyroid hormones accelerate bone turnover, decrease bone mineral density, and can lead to weak, brittle bones (osteoporosis) and fractures [9, 10].
Graves’ Disease and Cancer
Studies suggest that people with Graves’ disease may have a higher risk of certain cancers than healthy people. In a meta-analysis of 33 studies, Graves’ disease doubled the risk of getting thyroid cancer [11].
Additionally, in a cohort study of 25,000 patients, those with Graves’ had a higher risk of developing head and neck, liver, breast, prostate, and thyroid cancer [12].
Graves’ Disease and Hashimoto’s Thyroiditis
Unlike Graves’, Hashimoto’s occurs when an antibody blocks TSH hormone activity and causes damage to the thyroid gland.
After discontinuing antithyroid treatment for 5 – 10 years, 15 – 20% of people that recover from Graves’ can develop hypothyroidism due to Hashimoto’s. Although the exact cause is unknown, researchers think that antithyroid medication may contribute [13].
Graves’ Disease and Other Autoimmune Diseases
Scientists found that one autoimmune disease often increases the risk of getting another. In other words, people whose immune system malfunctions and attacks a certain tissue is more likely to then similarly malfunction and attack other tissues [14].
In a study (cross-sectional) of 3200 UK thyroid patients, around 10% of people with Graves’ also had another autoimmune disorder, such as [14]:
- Rheumatoid Arthritis
- Lupus
- Type 1 diabetes
- Pernicious anemia
- Celiac disease
- Vitiligo (loss of skin color)
One exception is an autoimmune disease called myasthenia gravis which very rarely occurs together with Graves’disease. Scientists are not yet certain why, but they think it may be because both diseases require a similar mechanism involving Th17 cells [15].
Treatment For Grave’s Disease
It’s important to work with your doctor to treat Grave’s disease as soon as possible. Untreated hyperthyroidism can have serious negative consequences. Your doctor will help zero in on a treatment that’s right for you.
Radioactive Iodine (RAI) Therapy
Radioactive Iodine (RAI) therapy uses radioactive iodine and can either be used after antithyroid medication or as the initial treatment for Graves’ and hyperthyroidism. RAI works by getting into overactive thyroid cells and destroying enough thyroid tissue to lower thyroid hormone levels [16, 4].
RAI doses differ for each patient and can differ for each treatment. However, studies suggest that a fixed RAI dose is associated with better response rates [16, 4].
Although RAI is relatively safe, pregnant women should not undergo RAI because it can damage the fetus. Additionally, RAI may worsen Grave’s ophthalmopathy and increases the risk of hypothyroidism (low thyroid hormone levels) [16].
Antithyroid Medications
Propylthiouracil and methimazole are two antithyroid medications that help treat Graves’. They block the production of thyroid hormones [4].
However, since they mainly inhibit thyroid hormone production and do not address the cause of the disease, patients can experience a high rate of disease recurrence [17].
While antithyroid medications are generally well-tolerated, their side effects also include stomach problems, muscle pain, and rashes. They might also cause agranulocytosis, or extremely low count of specific white blood cells [18].
Methimazole has fewer side effects than propylthiouracil, which can potentially cause liver disease and failure [4].
Propylthiouracil is preferred in the first trimester of pregnancy because methimazole has a slight risk of birth defects [4].
Studies suggest that better long-term results are achieved when the therapy lasts for over a year.
Beta-blockers
Beta-blockers are drugs that help reduce high blood pressure or treat heart problems. Using beta-blockers can help rapidly relieve some hyperthyroid symptoms, such as increased heart rate. However, they have no effect on thyroid hormone levels [4].
Thyroid Removal Surgery
Doctors usually recommend removing the thyroid or parts of the thyroid (thyroidectomy) if other treatments were unsuccessful, unsafe, or if the patient cannot undergo other treatments. Additionally, removing the thyroid can provide quick results in comparison to other therapies [18].
Pregnant women can undergo thyroid removal surgery to prevent damage to their fetus from antithyroid medication or RAI [18].
Patients who undergo thyroid removal surgery for Graves’ disease have a risk for bleeding and nerve injury. They are also at risk for hypothyroidism (low thyroid hormone levels) after the procedure [19, 17].
Other
Although these new treatments are promising alternatives to the three main therapies, no human clinical trials are available at the moment. It may take several years until these treatments are proven effective and safe in humans. We’ll keep you posted.
Human Monoclonal Autoantibodies
Monoclonal antibodies (Mabs) are made in laboratories from human immune cells and can help detect and/or stop harmful antibodies. One such Mab, can block thyroid-stimulating antibodies and may be able to prevent the effect on thyroid in Graves’ disease [20].
Small Molecule Antagonists
Various small molecules can act as antagonists and block TSHR (thyroid stimulating hormone receptor) activity. In human cells, NCGC00229600 and NCGC00161856 successfully blocked the TSHR [21, 22].
Treatment For Grave’s Ophthalmopathy
Mild symptoms may be managed with artificial tears and lubricants. Your doctor may recommend the following for more severe symptoms [23, 24]:
- Glucocorticoids, that can decrease inflammation
- Other immunosuppressants, such as cyclosporine
- Orbital decompression surgery, may help the eyes return to their original position, usually done when the pressure on the optic nerve endangers vision
- Corrective surgery for eyelid retraction and restrictive myopathy
- Radiotherapy
Symptoms of Grave’s ophthalmopathy don’t necessarily improve with treatment for Grave’s disease. They may get worse for a couple of months before they start gradually getting better.
Lifestyle and Dietary Changes
Three things you can do, in addition to treatment, that will help improve your symptoms and improve your health in general are:
- Eating a healthy, well-balanced diet
- Regular exercise
- Avoiding or managing stress. Remember stress can trigger or worsen Graves’ disease.
Avoid foods high in iodine, such as seaweed, and iodine-containing supplements. They may worsen hyperthyroidism. Work with your doctor to figure out what foods and supplements you should avoid.
Supplements
Few supplements have been studied in humans regarding their effects on hyperthyroidism. Discuss the following supplements with your doctor.
Remember, these supplements may improve symptoms, but won’t address the cause of the disease! None of these supplements should ever be done in place of what your doctor recommends or prescribes!
Always speak to your doctor before taking any supplements, because they may interfere with your health condition or your treatment/medications!
L-carnitine
Studies suggest that L-carnitine may be beneficial in improving symptoms such as nervousness, fatigue, and irregular heartbeat [25].
Glucomannan
An initial study of 40 hyperthyroid patients (including 30 people with Graves’disease) found that glucomannan when taken with antithyroid medication, reduced thyroid hormones more than antithyroid medication alone. However, the effect tended to disappear after about 6 weeks of therapy [26].
Ahnjeonbaekho-tang (AJBHT)
AJBHT is an herbal remedy that contains 8 medicinal herbs: kudzu, Chinese skullcap, gypsum, platycodon, Angelica tenuissima, Chinese cimicifuga, fragrant angelica, and Chinese licorice [27].
Some scientists are of the opinion that this herbal remedy may serve as an alternative for antithyroid medication.
In a study (clinical trial) of 22 Graves’ patients, published in 2008, AJBHT reduced T3 and T4 levels while it increased TSH [27].
However, there have been no other human studies since to confirm this finding, nor studies that look into long-term effectiveness and safety of this herbal mixture.
Graves’ Disease and Genes/SNPs
A combination of environmental and genetic factors affect a person’s risk for Graves’ disease. We know that because people who have a close relative with Graves’, have a higher chance of getting the disease [28].
Research suggests that the HLA genes may play an especially important role in Graves’. Although the exact mechanisms are unknown, there are some variants that have been associated with a higher risk of getting Graves’, such as DRB1*03 (in Whites and Blacks) and DPB1 (in Asians) [28].
The following SNPs and genes have also been associated with the risk of getting Graves’ [28, 29]:
- rs2476601 (PTPN22)
- rs1883832 (CD40)
- rs231775 (CTLA4)
- rs3087243 (CTLA4)
- rs2268458 (TSHR)
- rs2239610 (TSHR)
- rs7528684 (FCRL3)
- rs3761959 (FCRL3)
- rs11264798 (FCRL3)
- rs10489678 (FCRL3)
- rs1368408 (SCGB3A2)
- rs41295061 (IL2RA)


